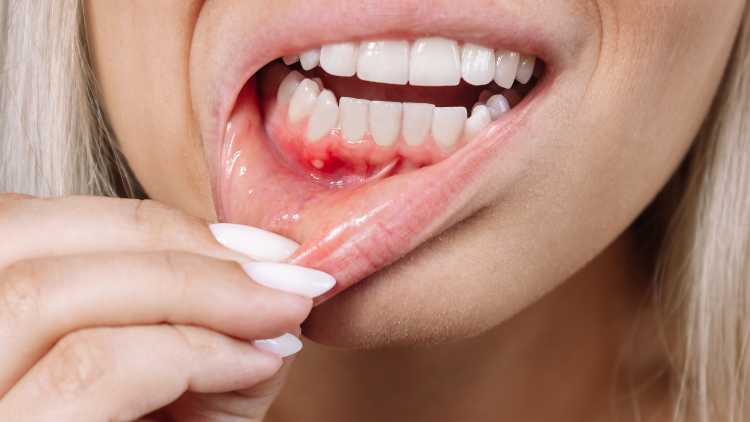
If you’ve noticed that your gums won’t stop bleeding, you’re not alone. Bleeding gums are a common issue that many people experience at some point. While it may seem like a minor problem, persistent gum bleeding can be a sign of something more serious and should not be ignored. In this blog, we’ll explore the possible causes of bleeding gums and offer practical solutions to help you restore and maintain healthy gums.
Common Causes of Bleeding Gums
There are several reasons why your gums may be bleeding. Some causes are related to your oral hygiene habits, while others could be connected to your overall health. Here are the most common causes:
1. Poor Oral Hygiene
One of the leading causes of bleeding gums is poor oral hygiene. If plaque—the sticky film of bacteria—builds up along the gumline, it can cause your gums to become inflamed and irritated. This can lead to gum bleeding, especially when brushing or flossing.
2. Gingivitis
Gingivitis is the early stage of gum disease and is often marked by red, swollen gums that bleed easily. It develops when plaque isn’t removed properly through regular brushing and flossing. Gingivitis is reversible with proper care, but if left untreated, it can progress into a more severe form of gum disease.
3. Periodontitis
When gingivitis is not addressed, it can lead to periodontitis, a more advanced gum disease. Periodontitis causes damage to the tissues and bone that support your teeth, which can result in loose teeth, persistent gum bleeding, and even tooth loss if not treated.
4. Aggressive Brushing or Flossing
Brushing your teeth too hard or using improper flossing techniques can irritate your gums and cause them to bleed. While it’s important to clean your teeth thoroughly, being too rough can do more harm than good.
5. Medications
Certain medications, like blood thinners, can make your gums more prone to bleeding. If you’ve started a new medication and notice that your gums are bleeding more than usual, it’s a good idea to talk to your doctor or dentist.
6. Nutritional Deficiencies
A lack of certain vitamins and minerals—especially vitamin C—can affect your gum health. Vitamin C helps keep your gums strong and healthy, and a deficiency can lead to gum bleeding and irritation.
7. Hormonal Changes
Hormonal changes, especially during pregnancy, can make your gums more sensitive and prone to bleeding. This condition is known as pregnancy gingivitis and typically subsides after the hormonal fluctuations stabilize.
When to Be Concerned
While occasional gum bleeding may not be an emergency, persistent bleeding is a red flag that something might be wrong. If your gums continue to bleed despite improving your oral hygiene, or if the bleeding is accompanied by other symptoms like pain, swelling, or bad breath, it’s important to see your dentist. Early detection of gum disease or other issues can prevent more serious complications down the road.
Solutions to Stop Gum Bleeding
Fortunately, there are several steps you can take to reduce gum bleeding and improve your oral health:
1. Improve Your Oral Hygiene Routine
The best way to prevent and treat bleeding gums is by maintaining a consistent oral hygiene routine. Brush your teeth twice a day with a fluoride toothpaste, floss daily to remove plaque from between your teeth, and use an antimicrobial mouthwash to reduce bacteria in your mouth.
2. See a Dentist for Professional Cleaning
If plaque buildup is causing your gum bleeding, professional cleaning by a dentist or dental hygienist can make a big difference. They can remove tartar (hardened plaque) that brushing alone can’t tackle and help you get your gums back on track.
3. Use a Soft-Bristled Toothbrush
Switching to a soft-bristled toothbrush can be a simple yet effective way to protect your gums. Soft bristles are gentle on your gums while still cleaning your teeth thoroughly.
4. Address Nutritional Deficiencies
Make sure you’re getting enough vitamins and minerals in your diet, especially vitamin C. Foods like oranges, strawberries, and bell peppers are rich in vitamin C and can support healthy gums. Consider taking a multivitamin if needed, but always consult with your doctor before starting any new supplements.
5. Manage Hormonal Changes
If hormonal changes are the cause of your bleeding gums, it’s essential to work with your dentist to develop a care plan that keeps your gums healthy. Extra dental cleanings during pregnancy or other hormonal changes can help manage sensitivity and bleeding.
Prevention Tips
Prevention is key to keeping your gums healthy and avoiding bleeding issues in the future. Here are a few simple tips:
- Schedule regular dental check-ups and cleanings.
- Brush and floss daily to keep plaque at bay.
- Eat a balanced diet with plenty of vitamins and minerals.
- Avoid smoking, which can worsen gum problems.
- Use a soft-bristled toothbrush and replace it every three to four months.
Conclusion
If your gums won’t stop bleeding, don’t ignore the problem. Bleeding gums can be an early sign of gum disease or other health issues, but the good news is that it’s often reversible with proper care. By improving your oral hygiene, visiting your dentist regularly, and addressing any underlying causes, you can take control of your gum health and prevent future problems.

 Request an Appointment
Request an Appointment